
The Need for a Faster Global Health Response
The West Africa Ebola epidemic can now see the light at the end of the tunnel. With over 22,000 cases and over 9,000 deaths, it is the largest Ebola outbreak since the virus was discovered almost forty years ago. The staggering loss of life in the region coupled with the destruction of families and communities is unfathomable. The importance of the wide media coverage and the large death tolls inflicted by Ebola is the lessons the local and international health organizations can learn from this.
In the months leading up to the World Health Organization declaring Ebola a full-fledged epidemic, the conversation centered around the lack of beds, medical personnel, international aid, and no centralized institution to direct relief efforts. The international aid that was visible did not come from official government sources but from non-profit medical organizations, such as Doctors Without Borders (MSF) and Samaritan’s Purse. These groups, comprised of mostly volunteer doctors and nurses, have spearheaded the effort to deal with the disease. From organizing themselves within the county to working with the locals, the effort against this multinational outbreak has been mostly led by volunteer groups.
Since the conception of the WHO and its predecessor, the Health Organization, there have been massive outbreaks across the globe that have captured the attention of the world. From HIV in 1970 to SARS in 2002 and Avian Flu six years ago; why does it seem that the response to a global epidemic has been reactionary rather than proactive?
Weak Local Health Systems
Epidemics have very small beginnings. Often they are in poor and isolated villages where the health systems are inadequate at best.
International health organizations rely on the response and open communication of the local systems to notify them about possible outbreaks of disease. A fundamental weakness that this past Ebola epidemic has exposed is the need for an improvement in the local level of health care across the world. Many of the deaths during the first few months were health workers. A nurse matron in Sierra Leone, Josephine Sellu, lost fifteen of her nurses in quick succession between June and July 2014. She is one of only three nurses left on the staff that have either not been infected or did not quite working at the hospital. By improving the effectiveness and relationship of public health within the local communities a more proper response can be mounted against diseases before it becomes an international problem.
Public Health Support
If there isn’t an epidemic, it is very difficult to argue for the need to spend money on public health systems. The urgency to raise money for events that haven’t happened yet, especially in health, is unfounded among the population and politicians. The unfocused attention to long lasting diseases, such as malaria, creates a new normal amongst health policy. The budget at the Centers for Disease Control, the United States de facto body on public health emergencies, was $6.6 billion for 2014; which is larger than the entire budget of the World Health Organization at $3.9 billion for both 2013 and 2014. Political and social disability is not only caused by conflict, health is an important part in the welfare of a country before, during, and after epidemics.
Adaptation as Diseases Occur and Lessons from Epidemics
Willingness to adapt is an important step as outbreaks occur and after epidemics have past. Viruses do not give warning to where or when they will become active. A part of having a fast and effective response to an outbreak as it occurs is to the ability to adapt and pull resources available to target the epidemic before it is able to gain a foothold in the population. The process of recognizing then treating the epidemic is too episodic. Treatment must be ready the moment a disease is recognized to prevent it from spreading. Geography, cultures, economy, and society are all factors that must be taken into account when dealing with global health policies. It isn’t only about preparing for outbreaks, using lessons from past epidemics in affected areas will help distinguish variables among societies that could be detrimental to the approach of treating future diseases. For example, efforts to treat Ebola during the early months of the epidemic were hindered by distrust of health workers and the customary practice of washing dead bodies. Understanding and adapting to cultural differences is essential to a decisive and quick end to epidemics.

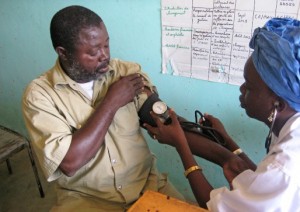





[…] The Need for a Faster Global Health Response […]